Causes and symptoms | Severity of the disease | Conservative treatment | Surgical treatment | After the treatment
Dupuytren’s disease is a benign disease of the palmar aponeurosis that most often affects the little and ring fingers. People may have a genetic predisposition to this disease and therefore the family history is important. Other causes such as diabetes mellitus, accidents, antiepileptic drugs or liver damage can also lead to growth of the palmar aponeurosis. Every year, 100,000 to 150,000 people in Switzerland experience Dupuytren’s disease. 60 to 80 per cent of people affected are men.
The layer of connective tissue in the hand called the palmar aponeurosis, is a complex, three-dimensional arrangement of longitudinal, transverse and deep fibres. The skin above it is connected to it by another layer, which forms the superficial fascia under the skin. The palmar aponeurosis is an important stabilising factor for the hand grip, as it enables close contact with the object being held without too much movement of the skin. It also protects the underlying blood vessels, nerves and flexor tendons.
Dupuytren’s disease usually develops slowly over a number of years. Over time, the function and performance of the hand can be impaired to such an extent that even simple tasks become difficult. Surgery is then usually required. At first benign, soft nodules form in the connective tissue of the palm. At a later stage of Dupuytren’s disease, fibrous cords can form along the finger tendons or flat scarring can appear. The fingers gradually become less mobile and full extension is no longer possible. Due to the deformation of the fingers, at an advanced stage it is no longer possible to lay the hand flat on a table, as shown in Figure 1. As a result, there is shrinking of the articular capsule, especially the middle joint. Tubiana’s staging system (see table) provides information about the severity of the disease. Other diseases that are related to Dupuytren’s disease and that can often occur at the same time are Ledderhose disease (the same formation of cords and nodules on the sole of the foot) and induratio penis plastica (affecting the connective tissue on the penis).
Stage 0 = No signs of disease
Stage N = Nodule formation
Stage 1 = Deficit of extension between 0° and 45°
Stage 2 = Deficit of extension between 45° and 90°
Stage 3 = Deficit of extension between 90° and 135°
Stage 4 = Total deficit of extension > 135°
The stages relate to the sum of all joint extension loss per hand.
TREATMENT OPTIONS
Conservative measures such as massage, ointments or exercises are not usually successful. For some years now, it has been possible to treat individual cords with a drug that is injected into the cord. The drug used is a collagenase clostridium histolyticum. However, this process can only be used for discrete cords and leads to the cord being dissolved. The nodules remain. In addition, the cords appear more frequently and earlier.
Another treatment option is the needling procedure. Individual cords are pierced with a needle under local anaesthetic until the cord breaks and the finger achieves better extension. X-ray treatment is generally no longer used because any success is very controversial.
Surgical treatment
Surgical treatment is still the most successful approach for advanced, complicated forms with nodule formation and severe finger deformation. The procedure is carried out under regional anaesthetic (anaesthesia of the arm) or general anaesthetic. A bloodless field is also created so that the surgery can be carried out without blood and under optimal conditions. The operation is carried out using a surgical loupe (magnifying glasses). The incision lines are made using a zigzag pattern from the palm of the hand and, if necessary, to the end joints. The skin is lifted off the nodules and cords. The vessels and nerves must be carefully removed from the connective tissue growths. The cords and nodules are removed as completely as possible. The articular capsules of the middle joints often need to be loosened.
With very severe deformation of the fingers, a skin defect may occur after full extension. In this case, skin flaps or grafts must be used for closure.
The procedure takes between one and two hours, depending on the severity and the number of fingers affected.
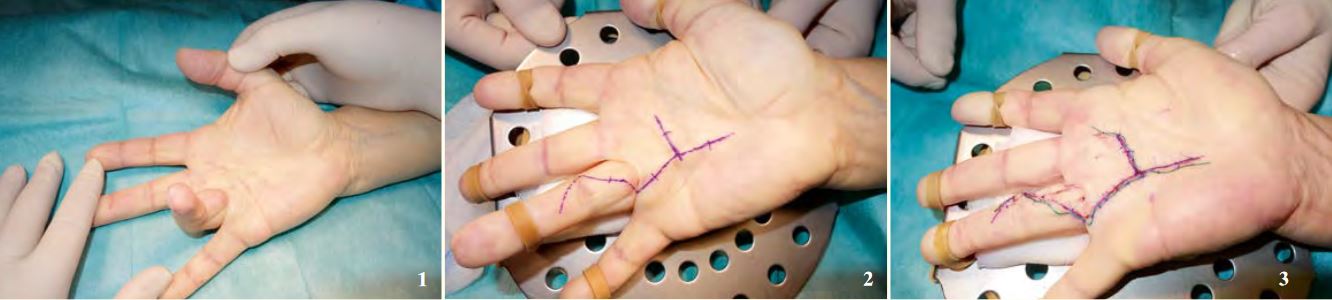
Figure 1: The ring finger can no longer be extended.
Figure 2: Before surgery.
Figure 3: After surgery.
A thick bandage is applied for a few days after surgery. This functions as a compression bandage to minimise bruising and has a “wicking” effect to absorb small amounts of blood. Active and passive mobilisation is begun very early, under occupational therapy guidance if required. After two weeks the stitches are removed and the hand can usually be used again without any major restrictions. Recurrence of connective tissue growth may occur and is more likely if a parent has also been affected, if the disease occurs before the age of 40 and if the index finger and thumb are affected. The risk is higher for women than for men. Despite this, Dupuytren’s disease is benign and can usually be treated well by an experienced hand surgeon.
Author: Dr Markus Strickler, FMH Specialist in Surgery, specialist field: Hand surgery
FACTS AND FIGURES
![SURGICAL PROCEDURE]()
SURGICAL PROCEDURE
1 to 2 hours, under general or regional anaesthetic
![SURGICAL PROCEDURE]()
HOSPITAL STAY
![AFTER THE TREATMENT]()
AFTER THE TREATMENT
Immobilisation for 5 days, removal of stitches after 2 weeks, joint splint for 2 to 3 months
![TIME OFF WORK]()
TIME OFF WORK
![Sport]()
Sport
![READY TO SOCIALISE]()
READY TO SOCIALISE
![COSTS]()
COSTS
Cost coverage must be requested from your health insurance company