Thyroid, parathyroid and adrenal surgery
Goitre | Thyroid nodules | Hyperthyroidism | Hypothyroidism | Thyroidectomy | Neuromonitoring | Thyroid cancer | Graves’ disease | Hyperparathyroidism
The range of endocrine surgery at the Pyramid Clinic includes thyroid, parathyroid and adrenal gland surgery. Complex findings are discussed with specialists in endocrinology, taking an interdisciplinary approach, and indications are assessed together.
Normal thyroid function
The thyroid gland is located below the larynx and surrounds the trachea. This small, butterfly-shaped organ fulfils a vital role, being responsible for the production, storage and release of thyroid hormones. These hormones regulate numerous metabolic processes as well as the energy balance of the body’s cells. If half the thyroid gland needs to be removed (hemithyroidectomy), the body’s supply of thyroid hormones is in most cases provided by the remaining half. Removal of the whole thyroid gland requires the use of hormone replacement therapy.
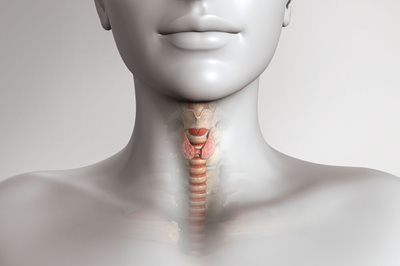 Fig.1: Location of the thyroid gland in the neck
Fig.1: Location of the thyroid gland in the neck
A goitre refers to an enlarged thyroid gland. In the past, goitre was very common in Switzerland due to a deficiency of iodine in the diet. Since iodine is a fundamental component of the thyroid hormone, iodine deficiency leads to a lack of effective thyroid hormone in the body. The body detects this deficiency and reacts by stimulating the growth of the thyroid gland. Uncontrolled thyroid growth or changes in the thyroid gland happen on a much smaller scale today. Sometimes the glandular changes are not visible and can only be felt by hand or possibly only detected by ultrasound. Nowadays these changes are interpreted as benign tumours of the thyroid gland, which are caused by mutations in the genetic material of the cells. Small nodules on the thyroid are common in young women.
If isolated nodules or lumps occur in the thyroid gland, these require further investigation. Formation of nodules in the thyroid gland is very common and is due to excessive production of thyroid hormone. This causes uncontrolled but benign growth of thyroid cells.
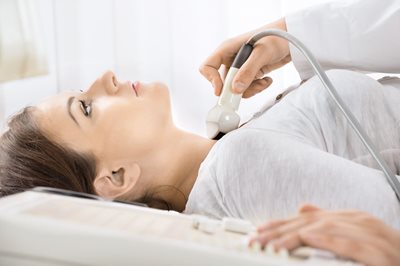 Fig. 2: Ultrasound examination of the thyroid gland
Fig. 2: Ultrasound examination of the thyroid gland
In the vast majority of cases, thyroid nodules are benign. However, as they increase in size and take up more space, these benign changes can displace neighbouring organs. If a malignant condition is suspected and if there are large nodules causing displacement, surgery is necessary.
The increased production of thyroid hormones by individual nodules (autonomous adenoma) or by the thyroid gland as a whole (Graves’ disease) causes an overactive thyroid. Typical symptoms include weight loss, a fast pulse and restlessness. In this situation, it is important for an endocrinologist to be involved in the treatment. Drug treatment to restrict the thyroid gland will be indicated. However, surgery is often necessary for definitive treatment of symptoms.
Hypothyroidism (underactive thyroid) is a deficiency of thyroid hormones, often associated with autoimmune disease or thyroid inflammation. This deficiency leads to various complaints such as fatigue, sensitivity to cold, constipation and muscle weakness. It is treated by administering thyroid hormones in the form of medication.
At the Pyramid Clinic, we currently offer conventional thyroid gland removal as well as the minimally invasive method. Both methods are safe and well proven. Minimally Invasive Video Assisted Thyroidectomy (MIVAT) is now the most widely used minimally invasive procedure in neck surgery. It is established as the preferred method for the removal of small thyroid glands and small nodules. Minor nodular changes of up to 2 cm in particular can be operated using a method that is painless, less invasive and cosmetically advantageous. Surgical access to the thyroid gland is achieved using the smallest possible horizontal skin incision to the neck of 2 to 3 cm.
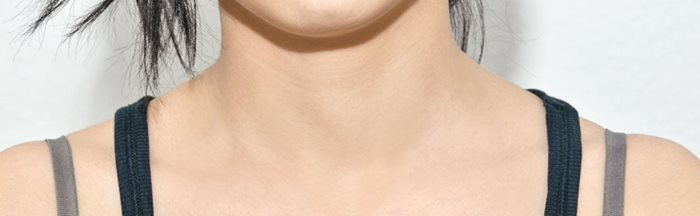 Fig.3: The reduction in incision length and placement of the incision in the skin creases mean that scars are practically invisible
Fig.3: The reduction in incision length and placement of the incision in the skin creases mean that scars are practically invisible
In order to carry out the surgical processes, the surgeon introduces an endoscope that provides an enlarged display of the area onto a screen. This reveals the parathyroid glands and the laryngeal nerve, enabling them to be protected during surgery. Minimally invasive procedures are not only cosmetically more favourable - the smaller the incision, the less pain the patient will experience after the surgery and the shorter the recovery period.
Using the latest generation of neuromonitoring (monitoring nerve function during surgery using electromyography), the risk of injury to the laryngeal nerves, which control vocal cord function, is reduced to a minimum.
Problems with temporary hoarseness after surgery can thus be significantly reduced. In order to avoid damage to the parathyroid glands, which are embedded in the surface of the thyroid gland, imaging is used during the procedure and care is taken to ensure there is no injury to their blood supply. The risk of postoperative hypocalcaemia is estimated based on a parathyroid hormone test on the first postoperative day and calcium substitution may be begun, depending on the result. Emergency readmission due to tetany (involuntary muscle contraction) can thus be eliminated.